Types of ovarian cancer surgery
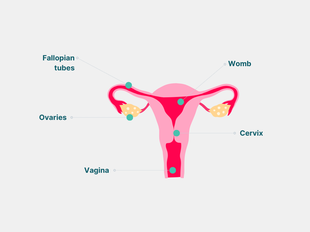
Reproductive system diagram
The type of surgery used to treat ovarian cancer depends on how far the cancer has spread. The medical team in charge of your care will discuss the best way to treat you, and your consultant will talk you through this treatment plan. They will explain the aim of surgery, what the operation involves, and answer any questions you have.
Here are some of the different ways surgery is used to treat early and advanced ovarian cancer.
Surgery to remove all of the disease
If you have stage one or two ovarian cancer, and it has not spread beyond the abdominal cavity, the aim of surgery is to remove all visible signs of the disease.
You may need to have one or possibly all of the following removed during the operation:
- The affected ovary and its Fallopian tube
- Both ovaries and Fallopian tubes
- The uterus (womb) and cervix
- Lymph nodes and surrounding tissue
- The omentum (a fold of fatty tissue covering the intestines)
The surgeon will check for any other signs of cancer. They may do this by doing carrying out a procedure called abdominal or peritoneal washing, which involves putting fluid into the abdominal area and testing it for signs of remaining cancer cells.
Surgery to remove the ovaries and womb
If your ovarian cancer has been diagnosed at a very early stage you may only need to have one or both ovaries removed. The operation to remove an ovary and Fallopian tube is called a salpingo-oophorectomy, and a bilateral salpingo-oophorectomy is when both ovaries and Fallopian tubes are taken out.
Most women will have their ovaries, Fallopian tubes, womb and cervix taken out during surgery. This operation is called a bilateral salpingo-oophorectomy (BSO) with a total hysterectomy.
When the ovaries, Fallopian tubes, and womb are removed during surgery, this will mean that you are not able to get pregnant naturally. There are steps you can take before starting your treatment that may preserve your fertility and enable you to have a family. If this is something you want to look into, have a conversation with your doctor before surgery and they will explain your options.
Surgery to conserve fertility
Fertility-sparing surgery involves removing the areas affected by cancer and leaving the woman with her womb and a healthy ovary. This type of surgery means that you are still able to have children naturally if that is something you wish to do.
It may be performed if the woman has been diagnosed with ovarian cancer at a very early stage (1a for example).
During the surgery a sample will be taken from the other ovary to check it’s disease-free. If there are signs of cancer, a second operation will be required to remove the second ovary and Fallopian tube as well.
It’s likely that your consultant will recommend removing your remaining ovary at a later date in order to reduce the risk of ovarian cancer returning. They should have a conversation with you about fertility options here as you may wish to conceive naturally or have your eggs frozen before the remaining ovary is removed.
Surgery to remove as much of the disease as possible
If your ovarian cancer is advanced, where it’s started to spread from the ovaries into other part of the body, the aim of your surgery will be to remove as much of the disease as possible.
This type of surgery is known as debulking surgery.
Sometimes debulking surgery is performed when, in theatre, the surgeon discovers that it’s not possible to remove all of the disease as originally planned because the cancer had spread further than expected. This can happen when the exact stage of the cancer is unknown prior to surgery.
Removing part of your bowel
In some cases women will have part of their bowel removed if the cancer has spread there. Wherever possible, the surgeon will only remove the section of the bowel affected by cancer and join the remaining, disease-free parts back together. This will leave the bowel able to function as normal.
When this isn’t possible, the surgeon may have to perform a colostomy. This operation brings part of the bowel up through an opening created in the abdomen called a stoma. A small pouch is placed over the opening to collect the waste passing through the digestive system. A stoma can be permanent or temporary. After the operation, a nurse will teach you how to look after your stoma. They will be there to give you information and support and answer any questions or concerns you may have.
For support about adapting to life with a stoma visit Colostomy UK’s website or call them on their 24-hour free helpline: 0800 328 4257.
You can also read Fi Munro's blog post where she writes all about her experience living with a stoma.


